Experimental Treatment Uses Targeted Radiation To Treat Advanced Heart Disease
Photo caption: Roland Filart, MD, speaks with heart patient Dewey Caldwell at the Orlando Health Heart and Vascular Institute. Caldwell’s condition had deteriorated to the point that treatment was no longer working when Dr. Filart presented an experimental treatment that uses precise radiation to treat advanced heart disease.
Radiation oncologists usually avoid the heart at all costs, but an emerging therapy targets the heart to correct arrhythmias.
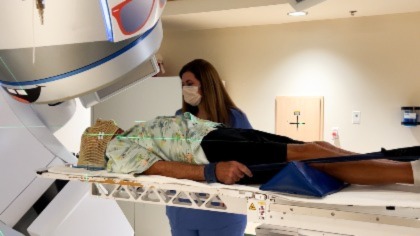
Orlando, Fla - Radiation oncologists rarely, if ever, treat the heart. In fact, they try to avoid exposing the heart to x-ray beams at all costs. But a new treatment performed at Orlando Health, using precise radiation therapy, has successfully given time and quality of life back to heart patients who have few, if any, remaining treatment options.
It began when cardiac electrophysiologist, Roland Filart, MD, and radiation oncologist, Justin Rineer, MD, realized they had read the same research about an experimental treatment for ventricular tachycardia, a rapid, uncontrolled heart rate triggered by a disruption to the heart’s electrical rhythm, often because of damage or scarring.
“We talked about whether this technology could be useful for a select number of our patients, and that's when Dr. Filart said, ‘Yeah, I have a patient in mind, and this could be a great choice to try to bring him out of this downward spiral of increasing tachycardia,’” Dr. Rineer said. ”We decided to begin this collaborative program and that Mr. Caldwell would be the first candidate."
Dewey Caldwell’s condition had deteriorated to a point that left him bedridden. He suffered more than two dozen heart attacks and, as his heart sustained more damage, there were fewer options to treat him.
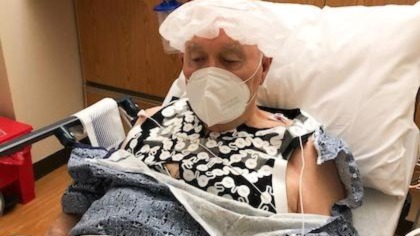
He got to a point where he was coming in and there were no blockages to clear or any other abnormalities other than the extensive damage to his heart,” Dr. Filart said. “With each episode, he got weaker and when medications were no longer effective, he underwent an ablation procedure. But that really took a lot out of him and he didn’t think he could go through it again.”
Dr. Filart implanted a defibrillator that shocked Caldwell’s heart when it fell out of a normal rhythm, but while it was keeping him alive, he was unable to do much without the device giving him a shock.
It was painful and the shock from the defibrillator knocked me to the ground on more than one occasion,” Caldwell said. “And it would go off when I really wasn’t exerting myself so I couldn’t do much of anything.”
Caldwell and his wife were planning to discontinue treatment when Dr. Filart approached them with a radical new option, explaining the targeted radiation therapy he had discussed with Dr. Rineer. The treatment uses stereotactic body radiation therapy, usually employed to precisely target tumors such as those in early-stage lung cancer that are between vital organs. But instead of avoiding healthy tissue, this treatment targets areas of the heart that are disrupting its rhythm and ablates them with a very fine beam of radiation.

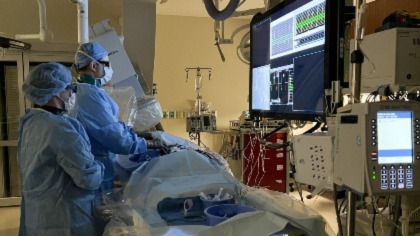
“We have never sought to treat the heart intentionally, but radiation technology can now pinpoint treatment within a millimeter, and we can use multiple different beam angles from all sorts of different directions to focus on a particular point in the body while avoiding sending x-rays through other parts that we don't want to treat,” Dr. Rineer said. “We focus a high dose of radiation to the exact spot that is disrupting the heart’s rhythm to basically change the way the heart functions and stop the arrhythmia.”
To prepare for the treatment, there is extensive planning and testing to translate cardiac heart mapping technology to work with radiation software and equipment.
“We monitor the heart’s electrical circuits and map the heart from all kinds of different angles and then we put all of those maps together, incorporate them into CT scans that our radiation oncology team uses and kind of overlay all of them to identify exactly where we believe the therapy should be targeted,” said Luis Garcia, MD, an electrophysiologist at Orlando Health. “
After months of planning, Caldwell received the radiation therapy, which took a total of about 30 minutes.
“It was a little anticlimactic,” Rineer joked. “He comes in, he lays down, this machine's moving around him, then he gets up and goes on with his day.”
“I came in and asked Mr. Caldwell, ‘How are you feeling?’ And he said, ‘Fine. Now what?’ And gets off the table and walks back to his wheelchair,” said Dr. Filart. “I told him, ‘That’s it! That’s your treatment.’”
In the weeks that followed, Caldwell’s energy dramatically increased and his defibrillator was deployed far less often.
“I got on a plane and went to my 60th high school reunion, which is something I never thought I’d be able to do,” Caldwell said. “My doctors never gave up on me and found a treatment that never even existed, but has made all the difference for me.”
The treatment that Caldwell received is still experimental and is only approved for compassionate use and not as a first line treatment. It is an option made possible through extensive planning and collaboration to translate cardiac heart mapping technology to work with radiation software and equipment. The treatment requires additional research to examine the long-term effects, experts are hopeful that it can help give many more patients more time and a better quality of life.
“We're doing radiation in a place that we usually try to avoid, so there's a lot of questions that we still have to answer,” Dr. Rineer said. “But for select patients that are really out of other treatment options, I think that this is a really valid treatment for them and one that can really be life-changing for the right patient.”
About Orlando Health
Orlando Health, headquartered in Orlando, Florida, is a private, not-for-profit healthcare organization with $8.1 billion of assets under management that serves the southeastern United States.
Founded more than 100 years ago, the healthcare system is recognized around the world for Central Florida’s only pediatric and adult Level I Trauma program as well as the only state-accredited Level II Adult Trauma Center in Pinellas County. It is the home of the nation’s largest neonatal intensive care unit under one roof, the only system in the southeast to offer open fetal surgery to repair the most severe forms of spina bifida, the site of an Olympic athlete training facility and operator of one of the largest and highest performing clinically integrated networks in the region. Orlando Health has pioneered life-changing medical research and its Graduate Medical Education program hosts more than 350 residents and fellows.
The 3,238-bed system includes 23 hospitals and emergency departments – 18 of which are currently operational with five coming soon. The system also includes nine specialty institutes, more than 100 adult and pediatric primary care practices, skilled nursing facilities, an in-patient behavioral health facility under the management of Acadia Healthcare, and more than 60 outpatient facilities that include imaging and laboratory services, wound care centers, home healthcare services in partnership with LHC Group, and urgent care centers in partnership with FastMed Urgent Care. More than 4,000 physicians, representing more than 100 medical specialties and subspecialties have privileges across the Orlando Health system, which employs more than 25,000 team members and more than 1,200 physicians.
In FY22, Orlando Health served nearly 142,000 inpatients and 3.9 million outpatients. The healthcare system provided more than $782 million in total value to the communities it serves in the form of charity care, community benefit programs and services, community building activities and more in FY 21, the most recent period for which this information is available. Additional information can be found at http://www.orlandohealth.com, or follow us on LinkedIn, Facebook, Instagram and Twitter @orlandohealth.




