Minimally Invasive Endoscopic Polyp Removal
As minimally invasive procedures used to remove polyps or lesions found on the surface of the bowel, endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD) offer patients a safe, effective treatment option with quicker recovery time than traditional methods. While most polyps of this kind are found in the colon, some are located in the duodenum (first or second part of the small intestine), stomach and esophagus.
With EMR, your endoscopist will insert a thin, flexible tube called an endoscope through your mouth or anus and guide it to the area of particular concern. EMR is used to remove large polyps — usually more than 15-20 millimeters in length. Once the polyp is located, a special solution mixed with dye is injected underneath the polyp to raise it up by lifting the mucosal layer away from the deeper underlying tissues. Your endoscopist will then use a cautery device called a snare to safely remove the polyp.
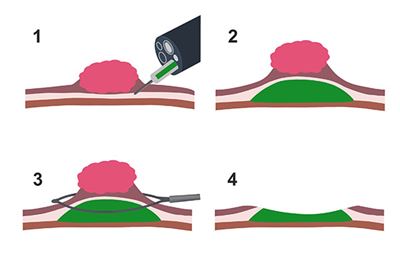
EMR
- Injection of a solution under the polyp
- Polyp is lifted
- Removal of polyp with snare
- Polyp is completely removed and collected for pathology evaluation
To remove lesions or polyps too large or located too deep for EMR, the advanced ESD technique, which is a longer and more complex procedure than EMR, is used. With ESD, the injection of a special solution mixed with dye is made into the deeper tissue layer, or submucosa, lifting the polyp or lesion. Using a device called an electrosurgical knife, your endoscopist cuts the submucosa and removes the lesion or polyp all in one piece.
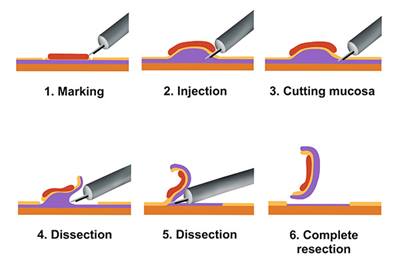
ESD
- Marking of polyp margins
- Injection of a solution to lift the polyp
- Cutting of mucosa
- Dissection of polyp by gentle cutting submucosa layer
- Dissection continues until polyp is completely removed
- Collection of specimen for pathology evaluation
Until recently, surgery was the only available option for the removal of these types of polyps or lesions, usually requiring a three- to 10-day hospital stay. Less invasive and less costly than surgery, EMR and ESD often can be performed as an outpatient procedure or with just one to two days of inpatient observation.
For EMR or ESD of the upper gastrointestinal (GI) tract, you cannot eat or drink anything (not even water) for about six hours prior to the procedure. Your doctor will give you specific instructions on when to start fasting.
For EMR or ESD of the lower GI tract, preparation will include either drinking a special cleansing solution or following a clear liquid diet in combination with enemas. Your doctor will give you specific instructions. If you do not precisely follow your doctor’s instructions, the procedure may have to be postponed.
Current Medications
Most medications can be taken as usual until the day of your procedure. Be sure to tell your doctor about all medications you are taking as well as any medication allergies that you may have. Anticoagulant medications (blood thinners) may have to be adjusted prior to the procedure. Warfarin (Coumadin) must be discontinued for five doses prior to the procedure; it can usually be resumed one night after. Clopidogrel (Plavix) must be discontinued for seven days before and five days after the procedure. Please contact our office for information on any other types of blood thinners you are taking. Sometimes, written permission from your cardiologist or prescribing physician may be required before stopping blood thinners or other medications.
If you have a latex allergy, please let your doctor know prior to the procedure so that any necessary precautions can be taken.
For EMR or ESD of the upper gastrointestinal (GI) tract, you will receive intravenous (IV) sedatives to help you relax. The procedure will most likely begin with you lying on your left side on the examination table. Once you are sedated, your endoscopist will insert the endoscope through your mouth and guide to the esophagus or stomach. You will be able to continue to breathe normally with the endoscope in place. Most patients find it to be only slightly uncomfortable, and many fall asleep during the endoscopic procedure. Likewise, if you require an EMR or ESD of the lower GI tract, you will be sedated and will not be aware of what is happening during the procedure.
Since you are sedated for the procedure, you will be kept in the recovery area and monitored until effects of the medication have diminished. If you had an upper EMR or ESD, your throat may feel a little irritated or you might feel a bit bloated because of air and water introduced during the procedure. You may experience slight abdominal pain, but that usually subsides with medication. You very likely will remain on clear fluids through the night following the procedure. You will be able to return to a normal diet the following day, unless your doctor instructs otherwise.
If you are not being admitted for an overnight hospital stay, you will not be allowed to drive after the procedure — even if you do not feel tired. Make sure you arrange for a ride home and someone to stay with you after the procedure; you may be feeling the effects of the sedatives you received for the rest of the day.
Normally, you will receive your EMR or ESD results the same day as the procedure. The lesion or polyp that was removed will be sent to pathology for microscopic assessment. These results will take about five to seven days and will be sent to your referring doctor. Depending on the results of the biopsy, you will need to follow up with us or with your referring doctor to confirm that the polyp or lesion is fully removed.
Occasionally, if a polyp penetrates deeper tissue layers, it cannot be removed with an endoscopic procedure. However, this can only be discovered during the procedure. In this case, you and your referring doctor will have to decide on treatment alternatives.
Standard endoscopy (or colonoscopy) is very safe. While rare, complications from endoscopic procedures can include:
- An adverse reaction to the pre-surgery bowel cleansing prep for colonoscopy or sigmoidoscopy, such as vomiting or headaches
- A negative reaction to the sedative given (This is very rare but is a concern for patients with severe heart or lung disease.)
- A puncture or tear in the gastrointestinal tract that may require surgical repair (Perforation occurs in about one of every 200 to 300 cases.)
- Major bleeding in the bowel caused by the endoscopic procedure (This can develop even up to seven days following the procedure.)
These possible risks must be weighed against the potential benefits of the EMR or ESD procedure and the risks of alternative approaches to your condition.

